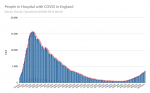
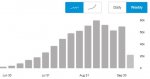
And here's how New Zealand conquered the virus
https://www.thelancet.com/journals/lanpub/article/PIIS2468-2667(20)30225-5/fulltext
Bolding mine..
New Zealand experienced one of the lowest cumulative case counts, incidence, and mortality among higher-income countries in its first wave of COVID-19 following early implementation and rapid escalation of national COVID-19 suppression strategies
New Zealand effectively achieved control with progressive, risk-informed border closures reducing the burden of imported disease driving the epidemic. This was followed, only 15 days after first case confirmation, by a phase of rapid escalation of non-pharmaceutical interventions to national lockdown. This 10-day escalation phase had the highest average daily case infection rate during the study period. Within 2 weeks, lockdown was associated with a substantial reduction in daily case infection rate and improving response performance measures: the majority of cases were detected by contact tracing, and there were decreasing average times to case notification and isolation and increasing population testing with effective targeting of higher-risk groups.
Enhancements in response capacity also supported de-escalation decisions. The daily test positivity was less than 5% from March 29 (day 4 of lockdown), as recommended by WHO before easing of restrictions, and only 25 cases of asymptomatic infection were detected despite routine testing of asymptomatic contacts, population testing surveys targeting asymptomatic and high-risk groups, and high testing rates by phase 5. Moreover, despite full de-escalation to Alert Level 1 on June 9, New Zealand effectively eliminated COVID-19, as currently defined to very low numbers detected at border quarantine facilities for an extended period.
Furthermore, rapid suppression of community transmission limited overall disease disparities for populations most vulnerable to severe outcomes. Most cases were linked to imported cases, with predominant features of healthy travellers: younger adults, European ethnicity, and higher socioeconomic status. Locally acquired disease was less common, but tended to reach more vulnerable populations (ie, older people, ARC residents, and minority ethnic groups) and was associated with more severe outcomes. Female case predominance in this group probably relates to the settings where locally acquired outbreaks occurred, including a girls' school, and ARC facilities where residents and carers were more likely to be female, but is potentially influenced by testing bias. Higher female testing incidence might reflect female predominance in certain high-risk groups targeted for testing, such as health-care workers, which is also considered a potential reason for slight female case predominance described in England.
Higher male mortality reported overseas was not seen in New Zealandand although the crude OR for severe outcomes was slightly higher for males, this estimate was imprecise and did not persist after multivariable adjustment. In keeping with some international findings, children appeared to have had a lesser role in household transmission and outbreaks—even at a school—in New Zealand, despite intensive testing of asymptomatic contacts.However, with lower national testing rates in children, detection bias cannot be excluded